Her body was itching, I thought it was an allergy!
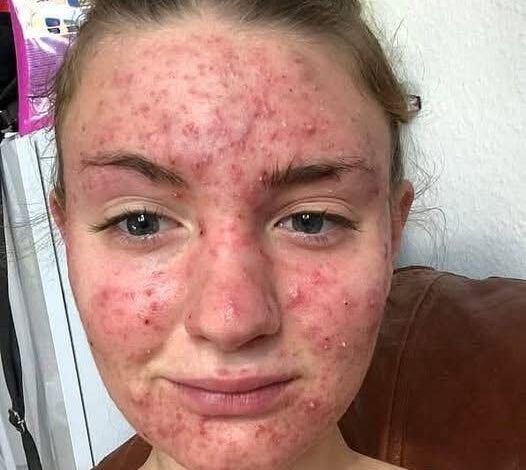
The human psyche is hardwired to seek the path of least resistance when confronted with the unexplained. We are biologically predisposed to favor the ordinary over the catastrophic, reaching for the least frightening explanation as a form of psychological self-defense. When my daughter first began to itch, my mind immediately constructed a fortress of mundane justifications. It was an allergy, I told myself. Perhaps a new laundry detergent, a change in the seasonal pollen count, or a reaction to a stray ingredient in a recent meal. It was far easier to believe in a localized skin irritation than to contemplate the possibility that her body was sounding a high-level alarm for a systemic crisis.
The progression was relentless. What began as a mild nuisance soon transformed into a wildfire of red patches that spread across her limbs and torso with terrifying speed. We embarked on the standard ritual of home remedies: antihistamines, cooling gels, and lukewarm oatmeal baths designed to soothe the surface. I rewashed every sheet and garment in the house with hypoallergenic soap, scrubbing away invisible irritants as if I could cleanse the problem out of existence. For a day, perhaps two, the fire would seem to retreat, offering a cruel glimmer of hope. Then, it would return with a renewed, sharper intensity.
The nights became a theater of quiet desperation. She scratched until the integrity of her skin failed, leaving behind a map of broken capillaries and raw, weeping welts. Sleep became a casualty of the condition. I would spend the early hours of the morning sitting on the edge of her bed, gently holding her hands to prevent her from hurting herself further. I whispered reassurances that I only half-believed, promising her that this was temporary, that it would pass, and that the morning would bring relief. But a deep, cold unease had begun to take root in my chest. This was not the behavior of a simple allergy. It was too aggressive, too persistent, and too resistant to the logic of over-the-counter medicine.
When we finally secured an appointment with a specialist, I walked into the clinic expecting a more potent prescription—perhaps a high-grade steroid cream and a calm, clinical explanation of a rare dermatological condition. The initial part of the consultation felt routine, almost dismissive. However, as the doctor observed the distribution of the rash and the texture of the skin, the line of questioning underwent a subtle, chilling shift.
The doctor stopped looking at her skin and started looking at her. “Has she been unusually tired lately?” he asked. “Any unexplained weight loss? Does she wake up with night sweats?”
The silence that followed was heavy with realization. I mentally replayed the last few months. Yes, she had been exhausted, but I had blamed the rigor of the school semester. Yes, she had mentioned feeling “off,” but I had attributed it to the growing pains of adolescence and the stress of her social life. I had contextualized every symptom of a systemic collapse as a byproduct of a busy life. The doctor’s expression shifted from professional curiosity to a guarded, careful focus. He ordered an immediate battery of blood tests and scheduled a series of imaging scans. In that moment, the exam room seemed to contract, the air growing thin as the reality of our situation began to crystallize.
Waiting for the results of a medical crisis is a unique form of torture. Time loses its linear quality, stretching into a heavy, suffocating weight. Every vibration of my phone sent a jolt of adrenaline through my system; every unknown number felt like a harbinger of doom. I spent those hours in a state of agonizing hindsight, replaying every moment I had dismissed her complaints, every time I had told her to just “stop scratching” or “try to sleep it off.”
When the clinic called and requested that we return in person to discuss the findings, the ambiguity vanished. I understood the gravity before the first syllable was spoken. The doctor sat us down and delivered the word with a gentleness that did nothing to soften its impact: Cancer.
Specifically, it was a form of lymphoma. The relentless itching, known medically as pruritus, was not the disease itself but a paraneoplastic symptom—a signal that her immune system was reacting to the presence of malignancy in her lymph nodes. The “allergy” I had been fighting with oatmeal and creams was actually her body’s desperate attempt to communicate that it was under siege from within. What I had labeled minor was the hallmark of a life-threatening emergency.
In the immediate wake of the diagnosis, a tide of guilt threatened to pull me under. I had promised her it would go away. I had minimized her suffering by calling it “just an allergy.” It is a natural human instinct to search for a focal point for blame when tragedy strikes, and I directed that blame squarely at myself. I questioned every delay and every assumption. But I eventually had to learn that illness does not provide the luxury of hindsight. It moves according to its own hidden rhythm, often camouflaging itself in the mundane until it is ready to be seen.
There was no time to remain paralyzed by shock or self-reproach. Our lives, which had previously revolved around school projects, social engagements, and minor domestic concerns, were abruptly reorganized. The new architecture of our existence was built from hospital corridors, laboratory results, and oncological treatment plans. The concerns that had felt urgent only a week prior—the upcoming exams, the broken appliance, the social drama—faded into a quiet, irrelevant background.
Looking back from the vantage point of 2026, a year already marked by geopolitical shifts and the high-stakes news of global military helicopters and international coalitions, I recognize that the most significant battles are often fought in the silence of a pediatric ward. I have come to understand that we prefer simple explanations because the truth is often too much to carry. Our instinct for the ordinary is not negligence; it is a fundamental part of the human condition. However, that instinct can act as a veil, delaying the clarity required to save a life.
The lesson we carried away from the itching is one of vigilance. Persistent symptoms that resist standard treatment are not to be ignored or explained away. Seeking a second opinion or asking “why” one more time is not a symptom of panic; it is the highest form of care. Calm, firm persistence can protect more than silence or false reassurance ever will.
For us, the nightmare began with an itch—a symptom so common it is almost invisible. It became a reminder to listen closely to the whispers of the body before they become screams. What changed our lives was not just the clinical diagnosis or the subsequent treatment; it was the realization that attention—deep, patient, and unwavering attention—is a profound act of love. When fear arrives, we must meet it with deliberate action rather than the paralysis of self-blame. We are now in the business of listening, responding steadily to the signals, and honoring the resilience of a body that, despite everything, found a way to tell us the truth.