THE TERRIFYING TRUTH BEHIND CIRCULAR RASHES Why That Red Ring On Your Arm Could Be More Dangerous Than You Think
The human skin is the body’s largest organ and its primary shield against the outside world, yet we often take its integrity for granted until something visible goes wrong. Finding a red, circular mark on your arm can trigger a cascade of anxiety, leading many to fall down a rabbit hole of internet searches and self-diagnosis. While some marks are harmless, others are persistent signals from the body that an invasive pathogen or an underlying inflammatory condition has taken hold. Understanding the nuances of these dermatological developments is not just a matter of aesthetics; it is a critical component of maintaining your long-term health and preventing the inadvertent spread of infection to those you love.
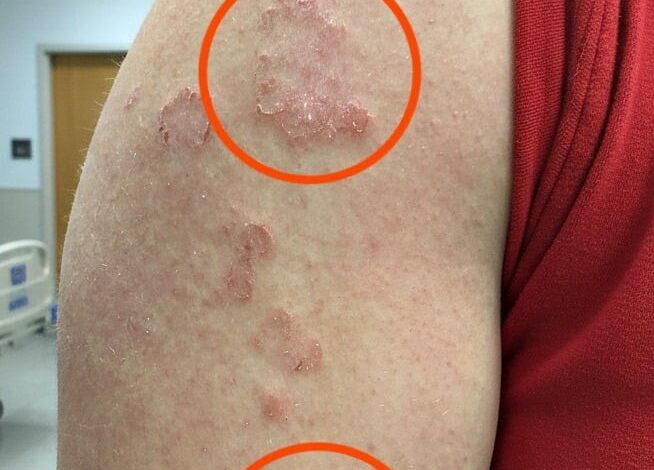
One of the most common and recognizable culprits behind the appearance of ring-shaped lesions is a fungal infection known colloquially as ringworm. Despite its name, this condition has absolutely nothing to do with actual worms. It is caused by tinea, a type of fungus that feeds on the keratin found in the outer layers of the skin, hair, and nails. When tinea takes root, it typically manifests as a red, itchy, and scaly patch. As the infection progresses, it clears in the center while the outer edge remains raised and inflamed, creating the classic ring-like appearance that gives the condition its name. These rings can slowly expand over time, claiming more territory on the skin as the fungus thrives on the body’s warmth and moisture.
The ease with which ringworm spreads is one of its most frustrating characteristics. It is highly contagious and can be transmitted through direct skin-to-skin contact with an infected person or even an infected pet. Many people are surprised to learn that their sudden skin irritation actually originated from the family dog or cat. Beyond direct contact, the fungus is incredibly resilient and can survive on surfaces for extended periods. Sharing towels, clothing, or bedding with someone who has the infection is a common route of transmission. Furthermore, public spaces like gym mats, locker room floors, and pool decks are notorious breeding grounds for tinea. Because the fungus thrives in warm, damp environments, it is particularly prevalent in areas where people sweat or where water frequently accumulates.
However, the medical reality is rarely as simple as a single diagnosis. Not everything that forms a circle on the skin is an infection. This is where the danger of self-treatment truly lies. Several non-contagious inflammatory conditions can mimic the appearance of ringworm with startling accuracy. Nummular eczema, for example, is characterized by coin-shaped spots that can be intensely itchy and scaly. Unlike ringworm, this form of eczema is not caused by an external pathogen but rather by an overactive immune response or extreme skin dryness. Similarly, certain types of psoriasis can manifest in circular patterns. These conditions are deeply rooted in the body’s internal chemistry and immune system, meaning they cannot be “caught” from another person, nor can they be cured with simple over-the-counter antifungal creams.
The distinction between an infection and an inflammatory condition is critical because the treatments are diametrically opposed. If a person mistakenly identifies eczema as ringworm and applies an antifungal cream, the rash will likely persist, leaving the skin irritated and the underlying inflammation unaddressed. Conversely, and perhaps more dangerously, applying a topical steroid cream—the standard treatment for eczema—to a fungal infection like ringworm can lead to a condition known as tinea incognito. In this scenario, the steroid suppresses the body’s local immune response, which might temporarily reduce redness and itching but actually allows the fungus to grow unchecked and deep into the skin. This can lead to a much more severe, widespread, and difficult-to-treat infection than the original small ring.
Because the visual cues of these conditions are so similar, professional evaluation is the only way to ensure a safe recovery. A dermatologist or general practitioner has the expertise to look beyond the surface level. In many cases, a simple physical examination is enough for an experienced doctor to spot the telltale signs of a specific condition. If the diagnosis is unclear, they can perform a quick and painless procedure known as a skin scraping. By collecting a few scales from the affected area and examining them under a microscope—often using a potassium hydroxide (KOH) prep—the medical professional can confirm the presence of fungal hyphae. If no fungus is present, the focus shifts to identifying the specific trigger for inflammation, such as an allergy, a reaction to medication, or a chronic skin condition.
Ignoring these marks or waiting for them to “just go away” is a gamble that rarely pays off. A fungal infection that is left untreated can spread to other parts of the body, including the scalp or the groin, where it becomes significantly more uncomfortable and harder to manage. It also increases the window of time in which you might accidentally infect family members, friends, or colleagues. On the other hand, allowing an inflammatory condition to flare up without proper management can lead to permanent changes in skin texture, chronic pain, and a significant decrease in quality of life.
The appearance of red marks on the arm should be viewed as a communication from the body. It is a request for care and a signal that the skin’s delicate balance has been disrupted. Whether the cause is a fungus picked up at the gym or a sudden flare-up of a latent immune issue, the path to healing begins with an accurate diagnosis. Modern medicine offers highly effective solutions for both infections and inflammatory diseases, but these solutions are only effective when applied correctly.
In a world where we are constantly bombarded with quick fixes and DIY health hacks, the skin remains a complex system that requires specialized attention. If you notice a ring-shaped rash that burns, spreads, or fails to respond to basic hygiene and moisturizing within a few days, do not reach for the nearest tube of mystery cream in your medicine cabinet. Instead, seek the counsel of a professional. By acting quickly and getting a confirmed diagnosis, you can stop the spread of infection, soothe painful inflammation, and restore your skin to its healthy, protective state. Your health is too important to leave to guesswork, and your skin deserves more than a temporary fix. Take the signs seriously, get checked, and protect your well-being before a minor mark becomes a major medical hurdle.